A woman in Singapore recently took to Facebook to complain about the standard of care rendered by Changi General Hospital for her terminally ill grandmother.
The lengthy post came on the heels of a previous complaint by local actor Laurence Pang in March, about how he was disappointed with CGH for not diagnosing his blocked arteries condition.
In response to the latest incident, CGH issued a statement and apologised on May 15, 2019, for the anxiety that the woman's family experienced.
In the midst of all this publicity, one National University Hospital front line worker has come out to defend CGH and shed light on what healthcare workers face.
Experienced NUH nurse defends CGH
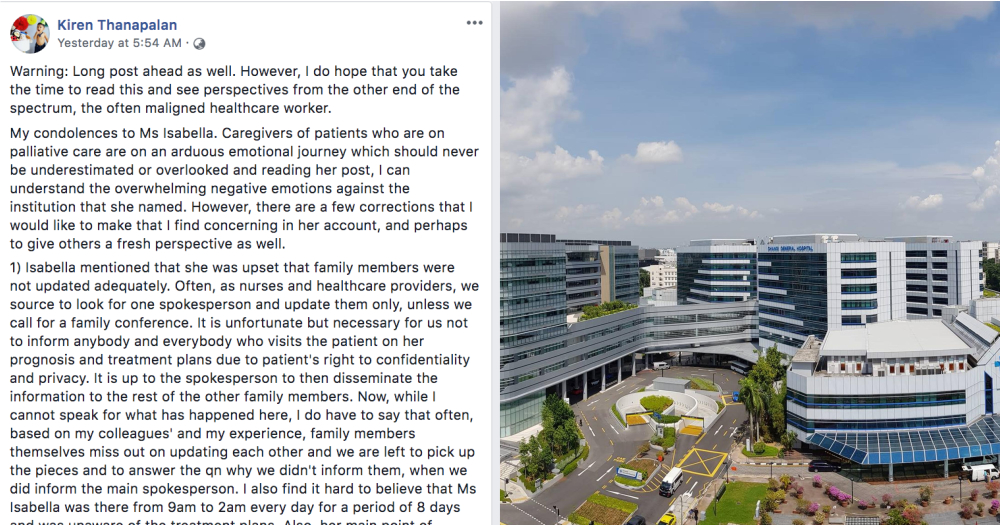
One nurse from NUH, Kiren Thanapalan, wrote a lengthy post on May 14, 2019 to share his perspective in defence of the healthcare workers at CGH in response to Isabella Lim's post about her grandmother.
In doing so, he hoped that members of the public can try to be more sympathetic towards healthcare workers in general.
According to Kiren, healthcare workers are trying their best to take care of the patients and have to prioritise their care-giving.
Kiren shared with Mothership.sg that he has been in the profession for seven years, and the only experience that he had in CGH previously was a four-week rotation when he was a student nurse.
When asked if NUH is systematically better than CGH, he said he does not think so:
"Honestly, I think that the system is always evolving to meet patient needs, and is probably as good as it gets already. I wouldn't say that NUH has a superior system to CGH.
Here's a summary of what he wrote.
Caregivers are involved in decision-making process
Kiren clarified that the healthcare workers in the hospital usually only inform one spokesperson representing the family.
The spokesperson is then responsible for disseminating information about the patient to the rest of the family members.
The healthcare workers will not be relaying information to every visitor on the grounds of patient confidentiality.
As such, it is important for family members to update each other promptly:
"Now, while I cannot speak for what has happened here, I do have to say that often, based on my colleagues' and my experience, family members themselves miss out on updating each other and we are left to pick up the pieces and to answer the qn why we didn't inform them, when we did inform the main spokesperson. I also find it hard to believe that Ms Isabella was there from 9am to 2am every day for a period of 8 days and was unaware of the treatment plans."
Kiren also highlighted that the administration of controlled drugs, such as morphine, do not require the consent from the patient's family and will be only be proposed if it helps to make the patient feel better.
He also explained that blood tests will not relieve any discomfort that the woman's grandmother was experiencing unless it is necessary.
"Isabella's contention is that the blood tests would have indicated an improvement and therefore a change in treatment perhaps? I highly doubt that would have happened. In a case of wants vs needs, I will be with the patient and be against unnecessary blood taking as well as they serve no purpose."
Communication can be better
As an observer, Kiren emphasised that he does not know how communication between the healthcare workers and Lim's family transpired.
But he concurred that doctors and nurses should be mindful and sensitive about communicating their views, as they might be misinterpreted because of inappropriate body language:
"Here, I do say that while the Dr might have just been explicitly stating a disclaimer that she is not familiar with Isabella's Ah Mah and she might need guidance and insights from caregivers who might know the patient best and can sometimes point out astute changes that might go unnoticed (like an increase in heart rate that was picked up by the family members and not the team per se), she had been misinterpreted as defensive and unprofessional. I do acknowledge that body language is key in non verbal communication and we can always do more as communicators and providers."
Moreover, doctors or nurses can be overwhelmed by the situation when they are caught off guard.
"I have to say that healthcare workers are often put in situations where they have to adapt."
"I have no excuses for the sigh, if that really happens, but I do have to say that large groups of people congregating can make professionals who are trying to assess a change in situation uncomfortable."
Palliative care is not just the nurses' job
In his post, Kiren also emphasised that palliative care is a collaborative effort between the caregivers and the nurses.
"This probably irked me the most out of her entire post. I'm sorry, but the general sentiment of 'we always had to wait, nurses had no initiative, we had to change diapers, do turning' doesn't sit well with me. It is a collaborative partnership, nurses and caregivers."
"Often, healthcare workers are portrayed negatively. Rarely are we praised online. This doesn't stop us from doing what we need to do as healthcare workers, pledging to giving our very best to the patients that we serve. However, what is a good enabler to us working to the best of our abilities are often caregivers who are good collaborators, who work hand in hand with us for the patient's best or their wishes. I wish that everyone who comes into hospital sees that, and not see us as just service providers. Healthcare is much more than that. We are much more than that."
In addition, he shared his observation that the helpers are often the ones taking care of the patients on behalf of the family members.
"These are the simple things that we want family members fully engaged in, and yet, often, we are seen as the maids who do these. The biggest regrets that some caregivers have in sudden demises are that they didn't do the meaningful tasks like sponging and diaper changes during the last moments of the patient."
He also suggested caregivers be more understanding of the nurses when they have to prioritise urgent cases and responsibilities.
"Also, you have mentioned that the nurses are nowhere to be found, maybe they are actually busy attending to more urgent needs? People often tend to lose perspective when admitted, we have to prioritise or we lose lives, simple as that."
"We do have to screen people coming in and it makes our job infinitely difficult if some family member takes prerogative to open doors just because they are irritated by the bell. If you find that that doors are not attended to promptly, give timely feedback. You have stayed there for 8 days or so, I hope that you at least spoke about the door to a nurse once and not rant it out about it."
He ends by making a disclaimer that what he shares are just his personal views.
You can read the full post here:
Top photo collage by CGH Facebook photo and Kiran ThanapalanIf you like what you read, follow us on Facebook, Instagram, Twitter and Telegram to get the latest updates.