“Do you think I’m fat?”
This is probably one of the most commonly asked questions of this generation. And a very tricky one for some to answer.
It is a tricky question because it isn’t really about wellness or health. More often than not, it’s about one’s attractiveness and how one looks. As such, one’s self-worth can be undermined when one is being described as “fat”.
The stigma of obesity can be dangerous.
It not only causes emotional and mental stress but also creates a psychological barrier for obese people to seek the help they need.
President of Obesity and Metabolic Surgery Society of Singapore, June Lee told Mothership:
“Social stigma may affect health-seeking behaviour, and individuals with obesity and poor mental health may shun treatment options for obesity, or develop maladaptive eating behaviours.”
Being fat can be an illness
So when does weight gain become a health problem? What’s the difference between overweight and obese?
Including Lee, we spoke with four local experts, two endocrinologists and two surgeons, to find out more about obesity.

Obesity is recognised by the World Health Organisation (WHO) as a chronic disease. What is diagnosed as chronic would be a medical condition that persists for a long time, just like chronic heart failure and diabetes.
When one’s Body Mass Index (BMI) hits 30 and above, one is considered obese, according to WHO, whereas one is considered overweight if their BMI is between 25 to 29.9.
Using the more substantial National Health Survey conducted in 2010, which involved 4,337 people, at least two in every five Singaporeans have a BMI of above 25, which puts them in the overweight or obese category.
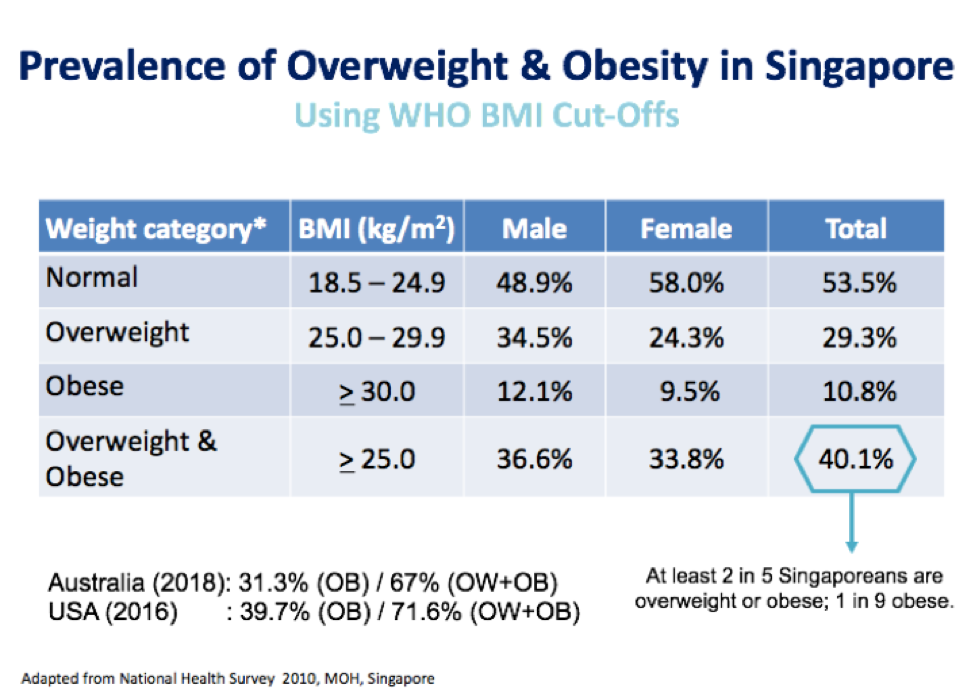 Image by Tham Kwang Wei, President of Singapore Association for the Study of Obesity.
Image by Tham Kwang Wei, President of Singapore Association for the Study of Obesity.
The prevalence of obesity is expected to increase from 10.8 to 15 per cent by 2024 because many Singaporeans tend to consume more than the recommended daily calorie intake.
While you might not mind having a “food baby” after a heavy lunch, you might not enjoy other “friends” that obesity introduces including diabetes, sleep disorders, heart disease, joint problems and infertility. These are known as comorbidities.
According to the WHO, there is a higher risk of these diseases with an increase in BMI.
Obesity can be genetic
More importantly, obesity can be caused by many factors.
People who are prone to obesity can gain weight easily from lifestyle and hormonal changes.
Genetic factors are also critical to one’s tendency to become obese as well, they pointed out.
If you have many family members who are obese, chances are it’s in the genes.
How so?
According to this 2012 medical paper, this means that you were born with a higher “set point”. In other words, your body will instinctively try to attain a higher level of body fat compared to others.
Because of that, many obese people face a harder time losing weight and sustaining that weight loss through exercise or changes in diet and lifestyle.
Similarly, they will find it easy to gain back their weight once they stop dieting or exercising as the body will return to that higher “set point” naturally.
Singaporeans could be at a higher risk of obesity
Tham Kwang Wei, who is the President of Singapore Association for the Study of Obesity, said that Asians tend to have a higher proportion of unhealthy visceral fat or “tummy fat” which is associated with obesity-related diseases as compared to an individual of Caucasian descent with the same BMI.
Adjusting the BMI cut-offs taking this factor into account, at least one in two Singaporeans would be considered overweight and obese, Tham added.
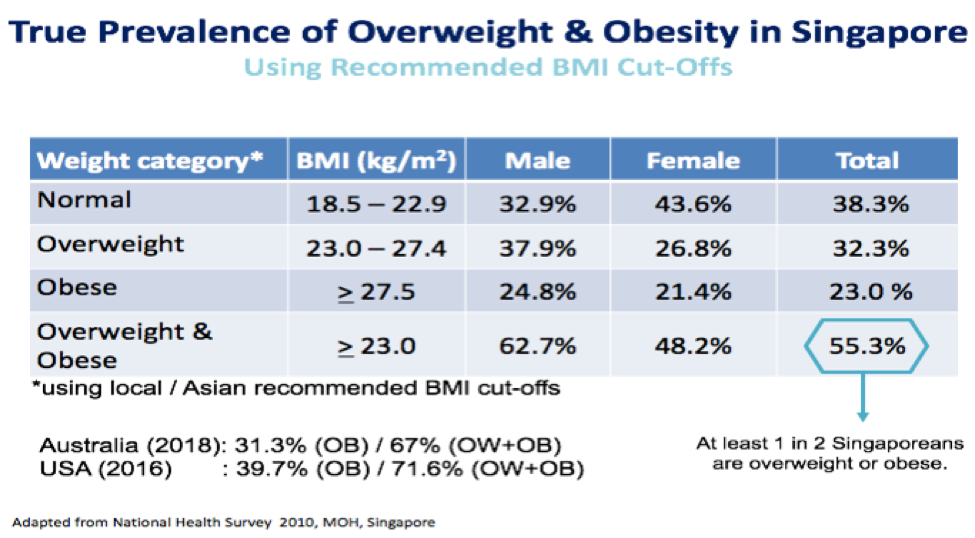 Image by Tham Kwang Wei, President of Singapore Association for the Study of Obesity.
Image by Tham Kwang Wei, President of Singapore Association for the Study of Obesity.
More than just the effort you put into losing weight
For a significant number of obese people, their condition is caused by genetic factors.
According to a 2011 study by the American Society of Bariatric and Metabolic Surgery, 95 per cent of obese people who lose weight with a rigorous weight loss program will regain their weight in two to five years’ time.
Evidently, for many obese people, their condition is wholly out of their control.
Therefore, social stigma against obesity is definitely unwarranted and might deter obese people from seeking proper medical help.
Ben Ng who is a senior endocrinologist at Arden Endocrinology Specialist Clinic said:
“The difference is that for obesity you can see it, I can see [the treatment is] not working for you. Blood pressure nobody knows. Therefore, there’s a stigma which we have to dispel. [Some might say],‘Oh you’re so fat that you need surgery because you cannot and nobody can help you.’ I think it’s very unfair.”
Lee also echoed the sentiment that obesity is more complicated than some might assume:
“Obesity is a complicated and multifactorial disease. Both genetic and environmental factors contribute significantly to obesity, and there is complex interplay amongst them. It is often mistakenly attributed to choice alone – whether from poor dietary choices, lack of exercise or willpower.”
Knowing your options
Those who suffer from obesity, morbid obesity, and other comorbidities, should seek proper medical help, experts urged.
There is no “one-size-fits-all” solution but there are many methods, treatments and programmes that have worked for different people.
What’s important is for individuals to know their health status, including fitness level before embarking on a dietary change, Tham recommended.
And safety comes first, Tham emphasised:
“Safety and first do no harm: remember, weight loss not the be-all and end-all but a means to an end which is to reduce the dire consequences of obesity be they psychological, social or medical.”
However, if you find it challenging to lose weight after multiple attempts, have pre-existing medical conditions like heart disease and diabetes mellitus, or gain weight rather rapidly, you are recommended to seek professional medical help from specialists.
Treatment for obesity usually involves a multidisciplinary team comprising medical specialists from different fields like endocrinology and surgery.
Medical therapy
The treatment process is consultative and can be customised according to one’s condition and depending on the severity of one’s obesity, said Ng:
“Like blood pressure, some people need four pills, some people need no pills, some people need to cut down salt — there’re a few variations of how you address this. In any chronic disease, some people would respond to diet management. Some people can lose 20kg that way and some people can’t.”
“Taking pills alone is not going to help you. Diet and lifestyle remain the pillar of therapy,” he added. #hardtruth
Patients undergoing treatment for obesity have to be disciplined in making adjustments to their lifestyle and to be consistent with their medication.
Bariatric surgery
In Singapore, morbidly obese patients are those of BMI ≥37.5kg/m2 with no other medical condition. These patients and those of BMI 32.5kg/m2 with an obesity-related medical disease such as type 2 diabetes mellitus, are eligible for surgical treatment.
While there are about 75,000 people who are morbidly obese, only 0.67 per cent have gone through bariatric surgery, senior consultant surgeon at Arden Jr Surgery Jaideep Raj Rao said.
500 bariatric surgeries were conducted in 2019, Rao added.
While there are risks involved — as per any other surgery — one should not be unnecessarily fearful of this treatment.
Rao and Ng said that surgical treatment could be a favourable option for severe cases while Lee said that patients who are deemed to have a low probability of success with non-surgical methods can consider such treatments.
“They must be aware of the risks and benefits of surgery and be highly motivated to comply with all dietary and lifestyle changes attendant to surgery,” Lee added.
So how does bariatric surgery work?
Bariatric surgery alters the anatomy of the stomach and sometimes the intestine. It basically reduces the food intake and also affects the production of certain gut hormones that interact with the brain to affect hunger and satiety, Lee explained.
It is a keyhole surgery (meaning it is minimally invasive) and patients can usually be discharged from the hospital after one to two days, according to Rao added.
Rao also pointed out that bariatric surgery aims to “cure” or reduce the comorbidities that a morbidly obese person has and can achieve a significant amount of weight loss, for instance, up to 50 per cent of one’s excess weight.
Altering the anatomy of the stomach also means that the body’s set point will change. Therefore, the weight loss can be sustained resulting in the remission of diabetes and other co-morbidities.
After the operation, the patient may not feel that hungry anymore as their hunger hormones are reduced.
That is when the doctor will have to remind them to eat low-calorie foods in small amounts regularly.
“The common misconception is that they don’t eat the whole day then eat heavy dinner. That slows down metabolism rate as the body conserves all the energy. Eat small amounts so the body burns faster,” Rao said.
Here’s a video that shows how bariatric surgery works:
Taking obesity seriously
Like all chronic diseases, the damage from obesity tends to creep in later in life and, before you know it, it is too late.
Obese women might find themselves struggling with infertility, obesity-related comorbidity.
Other obese people might find themselves developing various chronic diseases — such as heart disease, sleep apnea, and hypertension — that will impair their quality of life.
So it is important to recognise what causes obesity and how to deal with it, said Ng. And in the meantime, we should also recognise the challenges that obese people face and show them a little care and empathy.
Click here to learn more about obesity.
The writer of this sponsored article by Johnson & Johnson hopes to remind everyone that health is wealth and you are beautiful no matter what they say. Top photo via Pixabay.
If you like what you read, follow us on Facebook, Instagram, Twitter and Telegram to get the latest updates.
