Since the news of the Ministry of Health's (MOH) announcement of a cluster of Hepatitis C virus infections that saw 22 patients testing positive — of which eight have since passed on, half with their deaths linked to Hep C — both MOH and the Singapore General Hospital (SGH), the epicentre of the outbreak, have scrambled to account to a public demanding answers.
MOH announced on Oct. 6 that it convened an independent Review Committee to look into this, and its findings will be made public in two months.
The Terms of Reference of the Review Committee are "to provide an independent, objective and critical review of SGH’s report", to "identify the possible points of infection control breach", and "remedy any weak points in the overall workflow particularly with regard to infection control".
Here are five important questions on our minds (and possibly ones that you might have on yours too) we are looking forward to be answered in the review:
1. Why did SGH take so long to report the spike in Hep C cases to MOH?
According to a report by Today, between May to June, a total of 18 cases of Hep C was detected in SGH.
It was only in late-August, when the number of cases already rose to 21, that SGH informed MOH of an "unusually large cluster" of Hep C patients.
A MyPaper report by veteran health correspondent Salma Khalik quoted an internal SGH circular from the hospital's CEO, medical board chairman and chief nurse to its staff that said the delay was due to Hepatitis C not being an airborne virus — therefore announcing news of the spike in cases would "cause unnecessary alarm" and "that would not be responsible".
"We took action immediately in early June, when we noticed the clustering of seven cases within four weeks, which is unusual."
Did "action" in early June include turning patients away from the affected wards? Or were new patients still being warded in the affected wards? Could the cases of Hep C in July and August have been prevented?
We are also keen to understand which in the hospital's view is more important — (potential) patient safety and protection, or not "causing unnecessary alarm" to the public?
By the way, this Channel NewsAsia report (click the image above to go to the article) quotes SGH as saying they started contacting the infected Hep C patients and their families in the week of October 5. This, by the way, being more than a month after they finally informed MOH about the infected patients being part of a cluster in late August.
And here's another question: why were the other patients in the two wards and their families not informed earlier than October? Patients could then have made the call to be tested for Hep C and transfer to another ward or hospital to avoid infection.
Taking this even further, consider the fact that the eight patients who died before the news of this was announced would have passed away without even knowing that they were part of a cluster that, in all likelihood, would not have grown to the size it did if the hospital were up front about things earlier.
While we're on the topic of time lags,
2. Why did the MOH take so long to inform the public about it after hearing from SGH?
We trawled through the available material from both the hospital and the ministry so far to see if they have, eight days on from the first time they announced news of this, responded to this and question 1.
The closest thing we found was here:
 Screenshot from MOH website
Screenshot from MOH website
It would seem, from the above, that MOH's classification process of laboratory results would need further review.
It could well be the case, given this, that there was no way MOH could have found out without SGH informing them about their suspicions of the cluster.
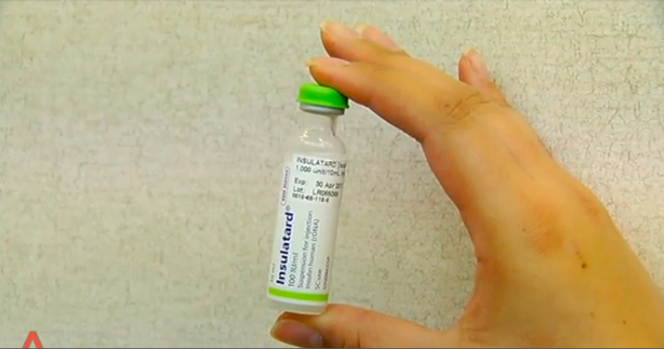 These multi-dose vials are suspected to be the cause of the virus spread. (Screenshot from CNA video)
These multi-dose vials are suspected to be the cause of the virus spread. (Screenshot from CNA video)
Their timeline indicates that SGH took four months from its first Hep C case to report an outbreak in its two renal wards, 64a and 67. MOH took a few days (until Sep. 3) to look over the hospital's report, then its director of medical services ordered that a laundry list of reviews and tests be carried out over the two weeks that followed.
After finishing them, the senior civil servant only informed Health Minister Gan Kim Yong about the infections on Sep. 18. SGH then took another week to prepare for a ministerial briefing, and then another full week to prepare to announce all of this to the press.
Now this might be understandable — for the governing body to confirm something like this is the biggest news in healthcare since SARS, possibly, and so of course everyone involved needs to tread super carefully and really be a million per cent sure of everything about it before going to town with it.
But still, it took more than four weeks between SGH informing MOH of the high number of Hep C cases in late August till the public announcement in early October. Does MOH view this as acceptable? Will this point be addressed in the review even though the committee is only looking at SGH's processes and not MOH?
Also, Minister Gan was only informed of the outbreak on Sep. 18, an entire week after the recently-concluded GE2015. But more importantly, why did it take MOH more than two weeks (between late Aug. and Sep. 18) to alert the Minister about something as serious as this?
3. Why were the bulk of potentially-infected staff and patients not screened for Hepatitis C prior to last week?
 Screenshot from CNA video
Screenshot from CNA video
We're glad the hospital did check the patients in the two wards at the time who showed abnormal liver function test results early on. We did notice, however, that it was only on Sep. 9 that the hospital started screening doctors and nurses who were directly involved in treating the patients.
Worse still, it was only from last week that they started calling back staff and patients who passed through Wards 64a and 67 for screening and tests. What if any of these hundreds of people (678 patients and 319 staff) happened to be carriers and unwittingly spread the virus through blood transfusions or donations, or treatments in other hospitals?
This links to our next question, which is:
4. Was contact tracing done to ensure all patients and potential carriers who might have been exposed to the virus have not passed it on elsewhere?
Was contact tracing done for the infected patients? This should be fairly straightforward — as has been stressed plenty of times, Hep C is not airborne, only transmitted by blood, so it should be easy enough for the hospital to find out if the 22 individuals had, upon discharge (where this had happened), donated blood or got re-warded elsewhere and received intravenous treatment.
If any of the above did happen, all the people who may have come into contact with the infected blood would most certainly have to be screened and in turn have their activities traced.
And finally:
5. How does the hospital plan to compensate families who lost their loved ones with reasons linked to this infection?
So far, infected Hep C patients reportedly said they were happy with the hospital's support provided to them and their families. But what about those who have passed away? These are eight lives gone that we can't get back — four of whose deaths were upon preliminary investigation found to be linked with Hep C.
A week ago, Prime Minister Lee Hsien Loong said at the official opening of Ng Teng Fong General Hospital (Oct 10) that the government approach to such incidents "must always be first to put things right, to find out what's wrong, to put things right, to safeguard the health and well-being of patients".
He added that the government "always (has) to be open and transparent with the public and with the patients about what has happened" because "we must maintain public confidence, and trust in the healthcare system".
Let's hope the independent review will shed some light on these questions when it is released in two months' time (again, what's with these extended timelines?).
Top photo from here.
If you like what you read, follow us on Facebook and Twitter to get the latest updates.
If you like what you read, follow us on Facebook, Instagram, Twitter and Telegram to get the latest updates.